Congestive heart failure. Arrhythmias. Cardiogenic Shock. Death.
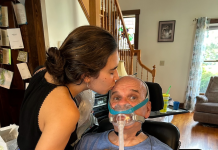
The words started to blur and swirl together while my throat tightened. My breathing became shallow and erratic until I collapsed into a dripping, whining, weeping mess. My hands shook as I typed in the same ten-digit number I’d memorized since childhood. The phone rang, and when my mom answered, I couldn’t stop the flood of sobs and snot—tears of sadness, but also of relief.
Chronic health conditions are no stranger to my family, largely due to limited healthcare access, low socioeconomic status, and low health literacy, among other barriers. Learning about diseases that have taken loved ones from my family has been an intimate part of my medical education. Yet somehow, this time felt different.
Reading through various lecture slides and looking at pictures of different heart deformities, I couldn’t stop myself from imagining that the patient in each case was my mother.
My mom survived three heart attacks, but in my cruel imagination, she passed away over and over and over from every post-MI complication we learned about. Each hypothetical patient we discussed became my mother’s ventricles dilating, my mother’s heart failing to pump blood to her organs, and my mother’s deformed heart on the examination table.
She doesn’t know. She doesn’t know all the ways that her body could betray her at any moment and take her away from us. She doesn’t understand why I bug her so much, reminding her to take her atorvastatin and metoprolol. She doesn’t realize the irreparable damage her heart sustained after one MI, let alone three. But I do.
They say knowledge is power, but sometimes it feels like a curse. It makes me fearful. It makes me overprotective, weighed down by the knowledge of just how fragile a heart can be. And it leaves me helpless, wishing I could protect her from threats she cannot see, from the many, many afflictions I now know to worry about for those who have already suffered an MI.
When my mom almost died in 2018, I was 18 years old. Despite her MIs occurring over 6 years ago, it wasn’t until last month that I truly understood the gravity of what my mom endured and survived. She told me she wishes she could share her story with people, so that’s why I’d like to share her story with you.
It was an ordinary day. My mom took a walk around her work building to escape her cubicle and close her Move Ring. When she got back to her desk, she felt short of breath. Feeling lightheaded, she took a seat, and then it started: a crushing chest pain she had never felt before. Her face flushed and she clutched her chest for an hour, enduring the pain without drawing attention to what she was going through. After sixty minutes of agony, it began to subside.
Nearly 24 hours later, to the minute, it happened again. This time, when she was simply sitting at her workstation. Again, my mom grit her teeth, put her head down against her desk, and quietly bore the agony alone.
“Susie, are you okay?”
She raised her head from her desk to see her boss standing over her, her face redder than a beet and her nose dripping with snot. Fortunately, a kind coworker realized the severity of her condition and drove her to the local Emergency Department.
She was triaged with the usual questions, had EKG leads placed, and underwent a physical exam. She described the crushing tightness in her chest, the difficulty breathing, and an odd tingling that started in her fingers and traveled up her arm. Yes, she’s up to date on vaccines, no history of childhood illness or trauma, blah blah blah-
Everything came back clear: no abnormal EKG, no abnormal labs, just a diagnosis of GERD based on her history of cholecystectomy. Thank god. Just heartburn. She was sent home with some calcium carbonate and acetaminophen as needed. Out of caution, she made a follow-up appointment with her primary care provider the next morning at 9 a.m.
On her way to work the next morning, she felt the familiar, ominous tingling in her fingers. She decided to go straight to her doctor’s appointment, arriving early at 8 a.m. She already knew the pain that would soon ensue.
“Sorry ma’am, your appointment isn’t until 9.”
My mom protested. “But I’m starting to feel this pain in my chest, it’s getting harder to breathe. Please, can anyone just give me something for the pain while I wait?”
“Please, take a seat until we call your name.”
For one hour, my mom suffered intense, crushing pain ALONE in the corner of the waiting room. For one hour, she clenched her head down between her hands, quietly crying, her face streaked with tears and snot, and bore through the pain until her name was called.
And when they finally called her name, she was too weak to even stand from her chair. She lifted her head from her hands, revealing a face flushed deep red, tears still falling from her eyes.
“Oh my god ma’am are you okay? You need to get to the Emergency Room NOW. Can you walk?”
Was she serious?
They wheeled her to the Emergency Department and waited for triage. When the front desk person saw her—
“Do you not see how much pain she’s in? Are you crazy standing in line like this?! Get her to the back room NOW!”
She was brought to one of those emergency emergency rooms, and the doctor hurried in and asked her questions while a tech placed EKG leads and took vitals.
“Has this happened to you before?”
She told him about the pain, the sobbing, the shortness of breath, the tingling over the last three days. As he examined the EKG, his eyes widened.
“Get MedEvac on the line!”
“MedEvac?” My mom was confused. “No, I’m fine, I don’t need that, save that for someone who really needs it.”
“Ma’am. YOU need it. You’re having a heart attack.”
My mom recoiled. “No, no, sir, I’m not having a heart attack, it’s just GERD, the other doctor told-”
“Ma’am.” The doctor sternly placed his hand on her leg. “You are having a heart attack.”
That was the first time she acknowledged what was really happening.
A whirlwind of people rushed into and out of her room, preparing her for flight, calling my dad, handling insurance, everything. The same front desk attendant from earlier rushed into her room, placed her hands on my mom, and said what my mom described as “the most beautiful prayer she had ever heard.” She was life-flighted to Shands Hospital at the University of Florida, my undergraduate university. While my mom was fighting for her life, I was probably in some monotonous chemistry class learning stoichiometry, unaware of what was happening a short distance away.
She says arriving at the hospital was like a scene from Grey’s Anatomy, with doctors in PPE rushing her into the OR. My mom loves that show. I like to imagine that someone like Cristina Yang was watching over her.
They performed what I would later learn to be a percutaneous coronary intervention to revascularize her left anterior descending artery, which is also colloquially known as the “widowmaker artery.” We learned how PCI access was achieved in the groin, and from there a catheter wound its way up into the aorta and eventually the coronary arteries to balloon out the blockage. What I didn’t know from class was that my mom was awake for the procedure. They were talking to her, trying to keep her cognizant. Lights in her face, needles poking and prodding her, and a group of strangers working vigilantly to save another stranger. She doesn’t remember much of the actual surgery.
She does, however, remember getting wheeled back to her room and the doctor checking in on her status.
“How are you feeling?”
“Terrible…like…I need to throw up.”
“What? No, you should be feeling good as new and so much better!”
“Please… get me a bucket.”
My mom “projectile vomited” into the pan immediately upon receiving it. The doctor’s face paled. “Call the OR we need to get her back in NOW.”
There had been a complication in her first surgery, an accumulation of fluid buildup around her heart—they thought they burst her coronary artery.
Fortunately, they didn’t.
My mom remembers arriving in the OR that second time, and once again, she says, it was like a Grey’s Anatomy scene, where the room was packed with observers trying to witness what was about to unfold. I guess it had to have been pretty bad. She remembers them inserting needles into various locations on her chest, struggling to get access to the pericardial sac. She remembers the pain. She remembers crying again, begging the doctors to anesthetize her.
“Please, doctor, please put me to sleep for this, it hurts so much. I’m in so much pain, you’re hurting me.”
“Ma’am we can’t put you to sleep—we don’t know if you will wake up. Please just keep talking to us, keep talking.”
She describes the sickening, grotesque sensation of fluid being drawn from her chest, how each gesture stole her breath away.
Eventually, she was wheeled out of the OR, awake and exhausted, but alive.
She was soon visited by the head of Cardiology at Shands, who told my mom that she had requested records from her ED visit and that her EKG clearly showed that she was having a myocardial infarction. Her first heart attack must have been the day before, after she had walked around her office at work. The doctor was furious that such a serious diagnosis had been missed. She promised my mom she would be taken care of from then on.
My mom is the strongest person I know. Like too many women, my mom’s “unusual MI symptoms” were misdiagnosed. She’s the epitome of resilience, surviving not just a heart attack but the oversight and misdiagnoses that nearly took her life.
Hearing my mother’s story changed everything I thought I understood about medicine. Her story taught me that every diagnosis, every misstep, and every overlooked symptom carries a human cost, one that isn’t always visible in small groups or exam rooms. Medicine to me is more than a career path—it is my mother’s life, my family’s history, and a source of both pride and responsibility. I came to understand that medicine is not only about preventing disease or saving lives but about listening closely, trusting the patient, and bridging the gaps that science alone cannot fill.
With her strength etched into my memory, I’ve made a promise to myself: no one in my care will ever feel unseen or dismissed. I want to be the kind of doctor who stays present through the suffering, who sees what lies beneath the symptoms, and who advocates fiercely for each patient. Her strength and resilience are now part of my own journey, empowering me to approach every patient with the empathy, attention, and vigilance they deserve.